Which Azoospermia is Treated With Medications?
Summary
A lot of Azoospermia patients visit us regularly and a lot of them have this common question, “Can Azoospermia be treated with medication?” So we decided to answer this question in detail via a dedicated blog.
In this blog, we will take a look at the condition itself, how it’s diagnosed and what treatment options are available for it. So let’s dive in.
What is Azoospermia?
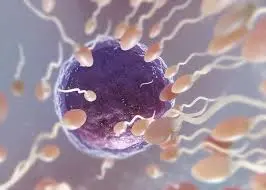
It’s a condition characterized by the absence of sperm in a man’s ejaculate, and it’s more common than many realize.
It’s a barrier to dreams of fatherhood for many couples.
In this blog, we’ll delve deep into what azoospermia means, the tests required for diagnosis, treatment options, and the crucial role of hormones in sperm production.
How Azoospermia is Diagnosed?
Before a path to treatment can be mapped out, a thorough diagnosis is crucial. Here are the foundational tests:
- Husband Semen Analysis: This test is the cornerstone of azoospermia diagnosis, assessing the presence or absence of sperm in the semen.
- Fallopian Tube Test: While this test focuses on the female partner, it’s part of a comprehensive fertility assessment for the couple.
If a semen analysis reveals a zero sperm count, the term azoospermia comes into play, and as Fertility doctors in Pune, we begin to consider our next steps carefully.
Types of Azoospermia and Their Treatments
Azoospermia can be divided into three categories:
Testicular Azoospermia refers to a condition where the testes are unable to produce sperm.
This could be due to genetic abnormalities, such as Klinefelter syndrome, infections like mumps that involve the testes, or damage from chemotherapy or radiation.
In these cases, the testes may be underdeveloped, atrophied, or damaged, directly impacting their function in sperm production.
Even if hormones are at normal levels and the rest of the reproductive system is intact, sperm cannot be produced or are produced in such low quantities that they don’t appear in the ejaculate.
Pre-testicular Azoospermia is related to hormonal or systemic issues rather than direct testicular function.
The testes may be physically normal, but they lack the hormonal signals needed to initiate sperm production.
Conditions like hypogonadotropic hypogonadism fall under this category, where there’s a deficiency in the gonadotropins LH and FSH, which are crucial for stimulating the testes to produce testosterone and sperm.
Other systemic conditions, such as severe illness or malnutrition, can also lead to pre-testicular azoospermia by affecting overall body function and, consequently, sperm production. This type of Azoospermia can be treated with medication.
Post-testicular Azoospermia is due to problems with sperm delivery. The testes produce sperm, but due to blockages or absence of the vas deferens (as seen in conditions like Cystic Fibrosis), or other obstructions in the male reproductive tract, the sperm cannot reach the ejaculate.
In some cases, ejaculatory duct obstruction can prevent sperm from being expelled during ejaculation.
Unlike the other two types, sperm are present in the testes, which means that they can often be retrieved directly from the testes or epididymis for use in assisted reproductive techniques like IVF or ICSI.
It’s important to note that not all types of azoospermia are treated with medication.
For post-testicular azoospermia, surgery may be necessary to retrieve sperm directly from the testicles.
Conversely, pre-testicular azoospermia can often be addressed with medications.
Hormones and Sperm Production
Understanding sperm production is crucial when treating azoospermia. Two hormones play pivotal roles:
- Follicle Stimulating Hormone (FSH): Essential for the creation of sperm within the testes.
- Luteinizing Hormone (LH): Helps regulate testosterone, which is crucial for sperm production.
For pre-testicular azoospermia, treatment may involve administering LH to stimulate testosterone production, followed by FSH injections to kick-start sperm production.
This hormonal therapy takes time—usually around 90 days to see results. The patient’s progress is monitored over 3 to 4 months to gauge the treatment’s success.
Treatment Outcomes and Assisted Reproduction
If sperm counts remain low, assisted reproductive technologies like Intracytoplasmic Sperm Injection (ICSI) come into play.
This procedure is a ray of hope for many couples, where a single sperm is injected directly into an egg, offering a chance at conception even when sperm counts are very low.
Conclusion
Azoospermia, while challenging, is not an end to the dream of building a family.
With the right diagnosis, a tailored treatment plan, and the advancements in medical science, many men with azoospermia have successfully fathered children.
It’s a path that requires patience, resilience, and trust in the medical process, but the outcome can be incredibly rewarding.
In closing, azoospermia is a complex condition, but with the wealth of medical options available today, it’s far from insurmountable.
Through a combination of hormonal treatments, surgery, or assisted reproductive technologies, there are a multitude of pathways to parenthood.

-
About Author
Dr. Supriya Puranik
Gynaecologist & IVF Specialist
MMC -072514 (1993)
Dr. Supriya Puranik, a renowned gynaecologist and infertility expert, leads the IVF & Gynaecology department at Sahyadri Hospitals Momstory in Shivaji Nagar, Pune. She is committed to helping couples overcome infertility challenges.
Appointment On Call





